A couple weeks back, Slate reported on Spurs forward DeJuan Blair and his lack of anterior cruciate ligaments. His situation is somewhat unique, as he didn’t have a traumatic event that took out the ACLs. Instead, it seems he had some partial tears in high school that progressed to full tears. Either way, he’s playing in the NBA without ACLs. He is a coper.
A couple weeks back, Slate reported on Spurs forward DeJuan Blair and his lack of anterior cruciate ligaments. His situation is somewhat unique, as he didn’t have a traumatic event that took out the ACLs. Instead, it seems he had some partial tears in high school that progressed to full tears. Either way, he’s playing in the NBA without ACLs. He is a coper.
The Arm Bone’s Connected to Our Future
Physical therapists are giving a hand and not in a good way. More and more, I’m hearing tales of PT settings where the PT sees exactly zero elbow, wrist, and hand patients. Those patients see the OT. Without exception.
Without exception, I find this deeply troubling.
The Daily Scallion: Secret APTA Task Force Seeks to Transform PT Branding
Most members of the American Physical Therapy Association know that their headquarters are well placed on the banks of the beautiful Potomac river in Alexandria. Most who are lucky enough to visit this strong hold never make it past the first floor conference room. The enlightened few can be escorted through the foyer into the inner sanctum, revealing grandiose views of the river, replete with expansive meeting spaces, all the splendor one would expect from a moderately funded professional organization.
What most people never see, however, is the bunker. The brainchild of APTA Treasurer and unofficial chief strategist, Elmer Platz, the bunker is accessed by a secret code in the elevator, and is located underground just east of the main structure. The bunker has periscopic windows, that are always spotless and offer a view of the river as well as escape routes, and a refrigerator full of several hundred containers of fruit-on-the-bottom yogurt. The design of the bunker, while impressive, is not the most captivating thing. What happens in the bunker, is. The APTA Bunker is the exclusive meeting location for every secret task force ever developed. While activities from secret task forces are well…secret, PTThinkTank.com has gotten exclusive access to information about one of these underground groups.
The super secret APTA Re-Brand task force has undertaken an interesting conversation.
TelePT: Inform Thyself

Day 65,000 of Shelter in Place (a.k.a 8),
There has been a heck of a lot of info flying around the airwaves as PT’s rapidly prepare themselves to be full on telehealth providers. I wanted to link to some resources:
- TeleHealth NOW Episode of Karen Litzy’s Healthy, Wealthy, and Smart Podcast. Featuring Mark Milligan from Anywhere Health.
- Recorded Live Webinar from APTA featuring Todd Norwood and Ellen Morello from Physera.
It’s a Strange, New World!
Well it’s been a bit. And what a bit it’s been!
I’m presently completing day one of “shelter at home” courtesy of COVID-19. As I am a regular worker from home, some parts of my day has not changed. Others, have changed greatly, and, really, who knows what is to come. I translate all this to: it’s a fine time to start writing again. Thus, new theme, new look, new images, and new thoughts for everyone!
Things on my mind:
- We waited too long to ramp up testing capacity
- CMS and HHS helped PT’s out today
- CDC is telling people what to do, not everyone is listening, or…to be fair, able to
- Biden WRECKED Bernie in FL tonight.
- Distance-based learning and education might become our new normal.
Stay tuned. I need to go fixed m “Y” button on m three week old MacBookPro which makes me ver angr .
#dumbcoronavirus #DCV
Priceless Protections: Pre-Existing Conditions Can Happen to You!
 Well, here we are again, on the cusp of another GOP vote on health reform, and about to lose federal protection for pre-existing health conditions. Troublingly, there has been this discourse floating around that places blame on said person with a pre-existing condition. As if, by making correct decisions, you can avoid having a need for health care, therefore, you should not have to pay for someone else’s care who made bad choices. This logic largely ignore rates of obesity and heart disease correlations to states where representatives (and constituents?) seem to think this way. Well, it’s wrong. Health, or the lack of it, is not a reflection of morality, or worth. Sometimes, and I know this personally, it happens in a split second.
Well, here we are again, on the cusp of another GOP vote on health reform, and about to lose federal protection for pre-existing health conditions. Troublingly, there has been this discourse floating around that places blame on said person with a pre-existing condition. As if, by making correct decisions, you can avoid having a need for health care, therefore, you should not have to pay for someone else’s care who made bad choices. This logic largely ignore rates of obesity and heart disease correlations to states where representatives (and constituents?) seem to think this way. Well, it’s wrong. Health, or the lack of it, is not a reflection of morality, or worth. Sometimes, and I know this personally, it happens in a split second.
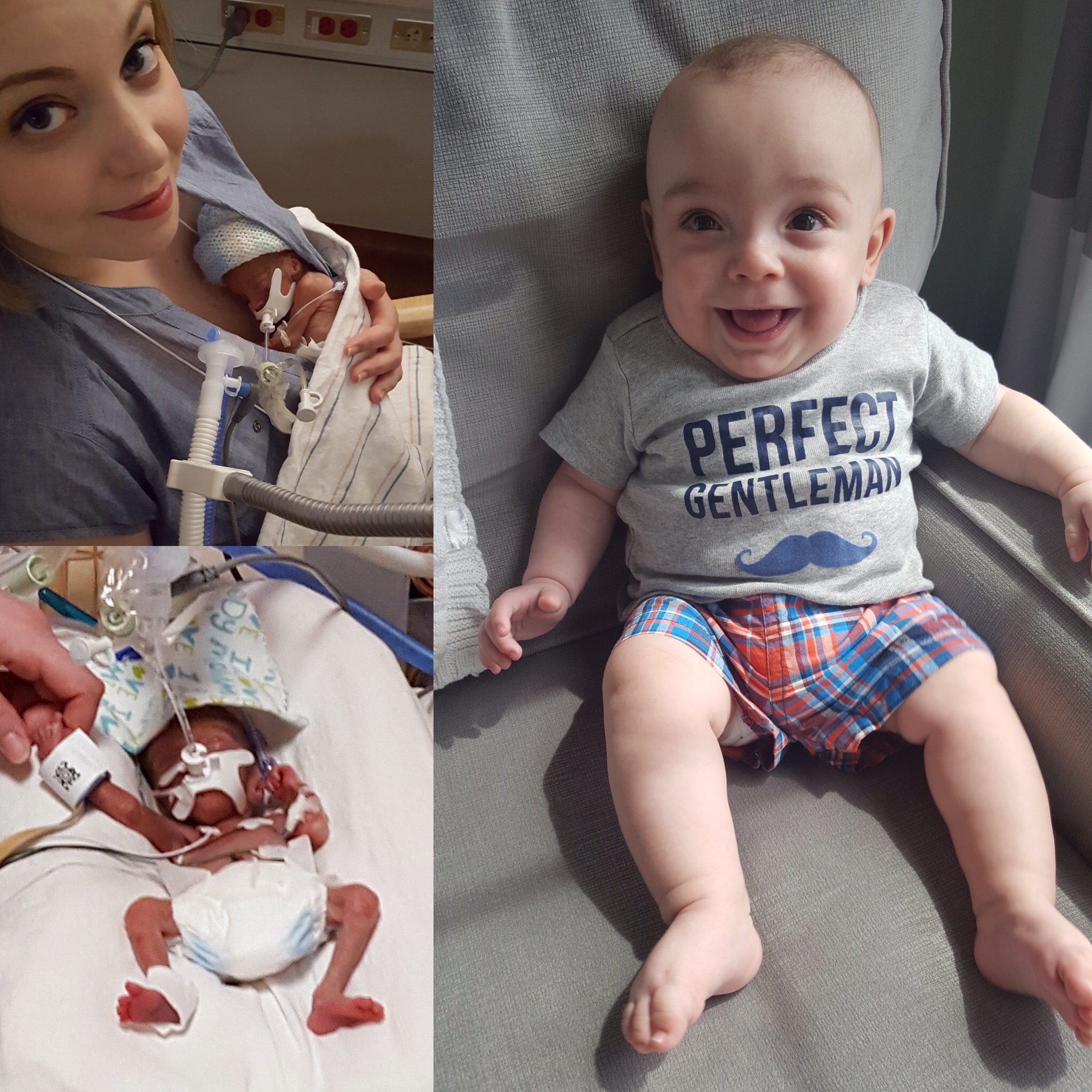
To illustrate this point, I’d like to share the story of a very dear friend of mine, Courtney Kelsch Ward and her family. Courtney posted this on her Facebook shortly after Jimmy Kimmel’s tale from Monday night. She was gracious enough to share. I think it illustrates the stark odds (and costs) in front of us as a nation as Congress decides to abolish pre-existing condition protection.
The Story of Baby Robbie
 On Monday night, Jimmy Kimmel gave a moving monologue in which he described the gut-wrenching experience of discovering his newborn son had a heart defect. Through tears, he explained the harrowing minutes when the doctors and nurses were examining his son in the neonatal intensive care unit, the ambulance transfer to a specialized hospital, and his son’s three-hour open-heart surgery. The story had a happy ending, thankfully, but Kimmel ended his talk with a plea for compassion and reason in healthcare reform.
On Monday night, Jimmy Kimmel gave a moving monologue in which he described the gut-wrenching experience of discovering his newborn son had a heart defect. Through tears, he explained the harrowing minutes when the doctors and nurses were examining his son in the neonatal intensive care unit, the ambulance transfer to a specialized hospital, and his son’s three-hour open-heart surgery. The story had a happy ending, thankfully, but Kimmel ended his talk with a plea for compassion and reason in healthcare reform.
Before 2014,” he said, “if you were born with congenital heart disease like my son was, there was a good chance you’d never be able to get health insurance because you had a preexisting condition. You were born with a preexisting condition. And if your parents didn’t have medical insurance, you might not live long enough to even get denied because of a preexisting condition. You can contact a reliable wholesale insurance company to solve all your doubts regarding insurance and help you out. If your baby is going to die, and it doesn’t have to, it shouldn’t matter how much money you make. I think that’s something that, whether you’re a Republican or a Democrat or something else, we all agree on that, right?
As it turns out, we don’t all agree on that. On Tuesday afternoon, former Illinois Representative Joe Walsh tweeted,
Sorry Jimmy Kimmel: your sad story doesn’t obligate me or anybody else to pay for somebody else’s health care.
Many others echoed this sentiment. An overwhelming number of people seem to actually believe that a baby deserves to die if his parents can’t afford to save him.
Over the last nine months, I’ve had a lot of conversations with a lot of people about the state of our healthcare system, and I’ve found one assumption lies at the heart of many of these arguments—that sick people have done something wrong to deserve their fate. A few days before Kimmel’s monologue went viral, Alabama Representative Mo Brooks said that increasing costs for people with preexisting conditions will help to reduce “the cost to those people who lead good lives, they’re healthy, they’ve done the things to keep their bodies healthy.” These are the people, he said, “who have done things the right way,” the implication being that sick people are those who have done things the wrong way. Back in January, Pennsylvania Senator Pat Toomey compared people with preexisting conditions to burned down houses. This belief is common. Not everyone says it as explicitly as these legislators, but deep down, many people hold this view—that good, hard-working, responsible people don’t end up in these situations.
I’m here to tell you, that’s simply not true.
My husband, Mike, and I approached starting a family the same we approach everything else—thoughtfully, with long discussions about logistics and preparation. We worked and reworked our budget and moved to the suburbs so we could get more space for our money. We bought books on how to have a healthy pregnancy and baby. I scheduled a mostly pointless pre-conception appointment with my doctor and took prenatal vitamins for the recommended three months prior to trying to conceive. When we finally got that positive pregnancy test, Mike wouldn’t let me lift a finger around the house. I stopped drinking wine, of course, and coffee. I even gave up my nightly cup of chamomile tea because I couldn’t find a clear answer about whether herbal tea is safe during pregnancy. I avoided unpasteurized cheeses and deli meats. I agonized over what to have for lunch every day, as even egg salad was questionable, according to the internet, as was really any cold meat. One time I asked the people at Panera to heat up the chicken on my Caesar salad, just in case. I suffered through chronic headaches because most painkillers are considered unsafe during pregnancy. My doctor said Tylenol was ok, but I avoided it anyway because a few studies have linked it to ADHD. I even started using different skincare products after deciding between a cosmetic dermatologist or surgeon because salicylic acid is considered possibly unsafe. The amounts absorbed when washing your face are minuscule, but over and over again, I asked: why take the chance?
All of this is to say: there’s doing things the right way and then there’s going way over the top, and we were certainly in the latter category.
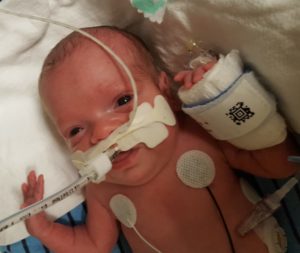
And yet, on July 25th, after just 22 weeks and 5 days of pregnancy, I went into labor. My doctors worked hard to stop the contractions and hold off my son’s birth, but four days later, on July 29th, my son was born at just 23 weeks and 2 days gestation. Some neonatal guidelines do not suggest intensive life saving efforts at this age. At 1 lb 5 oz and 11 inches long, Robbie was about the length of my forearm. His foot was half the size of my husband’s thumb. With severely underdeveloped lungs, he was unable to breathe on his own. A good outcome was certainly not a given. He was immediately intubated and remained on a ventilator for the first 78 days of his life. He spent over 4 months in the NICU, fighting to survive. There were many days when the doctors were not sure that he would make it. To this day, nine months after his birth, we consider it a miracle that our son is home with us.
We still don’t know why it happened. It wasn’t because of anything I did or anything I ate. It may have been because of something in my biological makeup, something that predisposes me to preterm labor. But maybe not. During my pregnancy, I had a single umbilical artery and slightly low levels of a hormone called papp-a. I would recommend you to avail therapy from http://www.swiftwatermedical.com/bioidentical-hormone-replacement-therapy/ to maintain hormone wellness. Both of these things increase the likelihood of preterm labor, but by such a small percentage that neither my OB nor the perinatal doctors were particularly worried. Neither of these factors were caused by anything I did, and the doctors said they varied not just from woman to woman, but from pregnancy to pregnancy. My OB herself told me she’d had low papp-a in her first pregnancy and completely normal levels in her second. The message from my doctors at the time was very much Do Not Panic. All of our other tests had come back good, so there was no need for alarm, they said. They planned to watch me a little more closely in the third trimester, but that was it. A second trimester delivery was not on anyone’s radar.
Since Robbie was born, we have asked why I went into preterm labor, why our son was born four months early, and we have received the same answer from every medical professional: sometimes these things just happen.
The cost of my week-long stay in the hospital was roughly $50,000. The cost of Robbie’s stay in the NICU was $1.7 million. This number does not include the costs since he has been home, the countless doctor appointments, the seven medications he was prescribed at discharge, four months of home nursing, three $3,500 shots to help protect him from RSV during cold season, or the oxygen tanks as noted by SimplyO3, currently sitting in my living room. No, that $1.7 million was just the cost of his 129 days in the NICU. It’s the cost of keeping my baby alive.
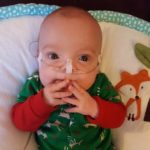
If our health insurance company had been allowed to set an annual limit to the amount they will pay for one person, Robbie probably would have hit that limit in 2016. If they were allowed to set a lifetime limit, he’d probably hit that too before long. Can you imagine looking at a nine-month-old baby and telling his parents he’d used up all of his healthcare coverage for his lifetime? We have been incredibly lucky in that Robbie is doing great and has made wonderful progress since coming home, but his prematurity puts him at a higher risk for a host of health issues, and Mike and I spend every day waiting for the other shoe to drop. The reality is, some day in the future, Robbie may very well be one of those people with preexisting conditions everyone is arguing about.
There are a lot of factors to consider regarding the economics of healthcare, and we have to continue having this complex debate. But we won’t be able to solve this issue as long as we think of sickness as something that happens to bad people who are lazy and irresponsible. When you pay for health insurance, you are not just paying for someone else’s healthcare. You are paying for the possibility that you, too, may need that care someday. Your education, your hard work, your moral superiority—none of these things can protect you from a health emergency or a chronic illness. You can do everything right and still end up in a hospital bed, or standing in a neonatal intensive care unit watching your child struggle to survive. It can happen to anyone. We could have been the spokespeople for “Doing Pregnancy Right,” and it happened to us. It can happen to you, too.
Dr. Manual Therapy, Or How I Came to Stop Worrying and Love the Placebo
With a central theme based on cinema, and a message potentially confused as a doomsday device for manual therapy, Dr. Joel Bialosky’s (along with Drs. Bishop and Penza) latest commentary in JOSPT, “Placebo Mechanisms of Manual Therapy, A Sheep in Wolf’s Clothing?” certainly deserves a Dr. Strangelove derivative title. But, is it really doomsday for manual therapy?
The fascinating thing about this must-read paper is the re-framing of placebo as a negative, non-specific sequitur of bad outcomes, to one of a specific, powerful, and necessary aspect of many interventions. To me, this is perhaps the key to how there can be so many different schools of manual therapy, and passionate adherence to each, and despite vastly different application, the apparent effectiveness of each. It’s as if we are all using different codes to access the same central computer, only to perform the same essential task.
The authors of this commentary leave us with a warning:
“Manual therapists, having invested large amounts of time perfecting their craft, may be troubled by the prospect of placebo as a primary mechanism.” Bialosky, Bishop, and Penza
I too, would like to issue a warning:
“The anti-manual crowd of therapists should also be careful to not mis-interpret the data around placebos by mistakenly believing this science is justification to not perform manual therapy.” Robertson
In a perfect world, the two groups would equally understand that specific active mechanisms of analgesia through physical therapy remain elusive despite the overall effectiveness of said treatment. Indeed, if we could work to understand the critical factors needed that result in a positive outcome for patients, perhaps we would be more effective at applying them, and less judgmental of people using a different coding set to access the “computer.”
Yet I wonder, what would happen to those practitioners stripped of their passion to defend their specific approach? Maybe that is the real doomsday device!
Chronic Whiplash: Is it really a Medical Mystery?
A small while ago, the well-known and widely read periodical, The Atlantic, published a piece entitled, Chronic Whiplash is a Medical Mystery.
In the article, the author, Julie Beck, poses the thematic question, “Being jostled in a car accident should only cause a few weeks of pain—so why do some people suffer longer?” Well, that is a good question, isn’t it? For many accident victims, the recovery process extends far beyond initial medical treatment, often requiring a comprehensive life care plan to address ongoing medical care, rehabilitation, and support services.
Over the past decade, tremendous advances in the science related to Whiplash and Whiplash Associated Disorders (WAD, as it were) have been achieved. Recently, this science took a giant step forward with the publication of Part I of a two-part special series dedicated to whiplash in the Journal of Orthopaedic and Sports Physical Therapy (October 2016 issue). This issue featured guest editors, Drs. Jim Elliott, Dave Walton, and Michelle Sterling and an editorial by Gwen Jull. Heavy hitters for sure. When it comes to accidents and injuries even if it is the ones that the injures in a truck accident on the highway there are lawyers to protect and get justice. People can check experienced moto accident attorney here if they need help with legal accident procedures. Injured in a car accident? The personal injury lawyers from Kogan & DiSalvo law firm can help.
Consult with a Racine truck accident attorney if you have been injured in a road accident involving a commercial truck. Contact the The Law Offices of Robert T. Edens to hire an attorney who will help ensure that your rights will be protected while filing a claim. Injured in Bakersfield? Call the personal injury lawyer from Johnson Attorneys Group.
So, it’s not surprising that some of these researchers took notice of Beck’s article in The Atlantic. It’s also not surprising that to these researchers, whiplash might not be the mystery it may seem to others. And so, without further ado, PTThinkTank.com is proud to publish a response piece to Beck’s article, entitled, “Chronic Whiplash: Is it really a Medical Mystery?” Well, that is a good question too, now isn’t it?
Enjoy the essay from Jim Elliott, Peter McMenamin, and Dave Walton. Thank you, sirs, for the contribution.
Putting Patients First: Man on a Mission
Decoding the Brain: Will Future Physical Therapists Manipulate Hippocampi Instead of Spines?
National Geographic Channel is featuring a slick new program:
“Breakthrough: Decoding the Brain” on Sunday, November 15, at 9 pm ET on National Geographic Channel.
As part of this show’s launch, they’re posing the following question for commentary:
“What if scientists were able to implant or erase memories? For some, like those suffering from PTSD this could be life-changing, or do you think this is scientific innovation gone too far?”
This question is right up our alley!
The Brain and Chronic Pain
The recent meeting of the American Academy of Orthopaedic Manual Physical Therapists (AAOMPT) in Louisville, KY was a bit unique. Unique, because in contrast to years and years of this conference unsurprisingly featuring scientists purporting the evidence for using manual therapy techniques like spinal manipulation for patients with musculoskeletal pain, this year the conference featured speakers who didn’t use their hands. The conference keynote was delivered by Dr. Peter O’Sullivan, (his cool blog is here) who spoke about his work related to Congnitive Functional Therapy for patients with chronic pain. Other talks revolved around pain science, big data, and a general change in the tenor was noticeable.
Manual therapists have long struggled with patients who have chronic symptoms, as short term gains are quickly realized, but long terms gains are extremely difficult to achieve. So, what prompted the AAOMPT, a scientific academy founded around manual therapy techniques, education, and science, to feature a pallet of speakers speaking about techniques that didn’t involve hands or cavitating joints? Well, friends, science is always a moving target, and it’s broad, and sometimes you need to look outside your cerebral solar system to learn new things. This is one of those times for physical therapists!
But, perhaps we don’t need to travel too far! This new traditional neuroscience science is now showing up in manual therapy journals like…well, Manual Therapy! In a recent article, entitled, “Exercise therapy for chronic musculoskeletal pain: Innovation by altering pain memories,” Nijs et al address the concept of movement-related pain memories and exercise for patients with chronic pain. They suggest that clinicians should preempt exercise therapy by first priming the brain via neuroscience education, and then utilizing movements to help the body ‘forget’ those memories associated with those movements and pain. Sounds just like Peter O’Sullivan’s CFT doesn’t it? This work builds on work by neuroscientists who are exploring the role of the hippocampus in generating pain-related memories. This is a wide open field, and the potential of learning how to impact pain related memories is truly astonishing!
Manipulating Hippocampi?
While the concept of having memories erased seems on the surface frightening… (I wouldn’t want to forget that cool downhill bike ride down Mount Snow even though it hurt!)… it does seem that breaking links between pain experiences and memories is one of the keys to managing chronic musculoskeletal pain conditions. Just how we do that best remains to be seen! Will future physical therapists have a cadre of tools that not only allows for mechanical inputs to alter central nervous system activity (spinal manipulation), but also precise strategies to target pain memories and more directly impact cognitive reasoning about pain? I sure hope so!
I’m excited for the new Breakthrough series on NatGeo. It just seems like one of those times when all sorts of science is converging on something…on the true potential of that “3lb mass in our heads!”