A couple weeks back, Slate reported on Spurs forward DeJuan Blair and his lack of anterior cruciate ligaments. His situation is somewhat unique, as he didn’t have a traumatic event that took out the ACLs. Instead, it seems he had some partial tears in high school that progressed to full tears. Either way, he’s playing in the NBA without ACLs. He is a coper.
A couple weeks back, Slate reported on Spurs forward DeJuan Blair and his lack of anterior cruciate ligaments. His situation is somewhat unique, as he didn’t have a traumatic event that took out the ACLs. Instead, it seems he had some partial tears in high school that progressed to full tears. Either way, he’s playing in the NBA without ACLs. He is a coper.
Do you have the resources to perform your job? #sportsPT
Matt Sremba, PT, DPT, OCS authored this guest post. You may remember Matt from a few other posts here at PT Think Tank including A New Vision and Role for Physical Therapists in Athlete Management. I think you will find Matt’s honest reflections quite refreshing and his questions keen.
@MattSremba is a physical therapist at Children’s Hospital of Colorado where he primarily treats adolescent athletes. He also serves as a physical therapist with Conatus Athletics. Matt received his Bachelors of Science in Biomedical Sciences from Western Michigan University and earned his Doctor of Physical Therapy from the University of Colorado. Matt is avid thinker, question asker, and non-accepter of the status quo. He has also been known to ride two wheeled objects and hike up inclines.
Do you have the tools and resources to do your job?
Have you been asked this question? How do you answer it? I explored this question at CSM 2015 in Indianapolis as the first speaker on a panel discussing Science, Technology, Engineering, and Math (STEM) and Physical Therapy: The Future of Sports Medicine. I believe examining this question will help us determine the vision and path for the future of sports medicine and physical therapy.
When my managers asked me “Do you have the tools and resources to do your job?”, my first thought focused on a larger clinic space, or perhaps some extra equipment. However, at some point, I started to ponder this question seriously. And I concluded, in order to determine the tools and resources I needed, I first had to re-examine a more fundamental question…
As a sports medicine physical therapist: What is my job?
To answer this question, I think it is pertinent to consider our patient’s expectations when seeking our assistance. My patients all come to me asking nearly the same questions:
1. What is the diagnosis?
2. Why did this injury happen?
3. How do I prevent this injury from happening again?
4. How do I get back to playing sports or activity?
Assuming this list makes up a significant percent of my job responsibilities, the question really becomes:
Do you have the tools and resources to successfully meet your patient’s expectations and answer their questions?
What do you think? Do you? My answer is: maybe. Sometimes I’m confident I can answer these questions. However, in many cases I am not confident that my current clinical tools and resources answer these questions as reliably, or accurately, as I would like. Lets look closer at one of these questions that all sports physical therapists are asked on a daily basis:
How do I return to sport?
Return to sport is a very challenging assessment and decision. I find it difficult to answer patient questions of: When can I run again? When can I cut again? When can I play basketball again?
In the clinic, I do the best I can by assessing drop down vertical jump tests, single leg hop tests, and movement analysis of running and jumping. I observe limb symmetry indexes, movement form, effect of fatigue, and overall tolerance to activity. However, I find these decisions very challenging.
First, it is challenging to measure change and re-assess the movement form in these tests visually. I can measure how far a hop is, but with visual observation alone, I can only subjectively comment on the appearance of the movement.
Second, these tests bring up many questions for clinicians. I’m left wondering: What am I looking for when I watch someone move? More specifically, how do I accurately analyze human movement?
I know that I need to look at strength. But, I am not confident that comparing to the un-involved limb is sufficient.
I know I need to look for shock absorption. But, what is shock absorption? What makes it good or bad?
I know I need to look for knee valgus. But what is normal knee valgus? What is an acceptable knee valgus angle to return to sport?
Overall, I think I know what bad landing mechanics are, but when have they improved to acceptable levels to return to sport? What are good landing mechanics?
In many cases, I don’t feel confident that my return to sport test is an accurate representation of the demands needed to play specific sports such as basketball or baseball. I need help because I know I can only answer, ‘are they ready for sport?’ if I truly understand the requirements and demands for that activity. For example, what are the requirements on the knee during basketball? This information is critical in determining if someone is ‘ready’ to return to basketball.
Who can help us answer these questions? Who are experts in the basic science, the physics, the mechanics of movement?
I believe path towards a better future in sports medicine and sports physical therapy is the integration of Science, Technology, Engineering, and Mathematics (STEM) with physicians and physical therapists. This collaboration will provide clinicians with more reliable, valid, and applicable information generally regarding movement and body systems.
Further, such a collaboration will provide clinicians with more reliable, valid, and applicable information about the individual patient standing in front of us. This will improve our ability to measure, assess, and progress. And, ultimately meet the goals and answer the questions of our patients.
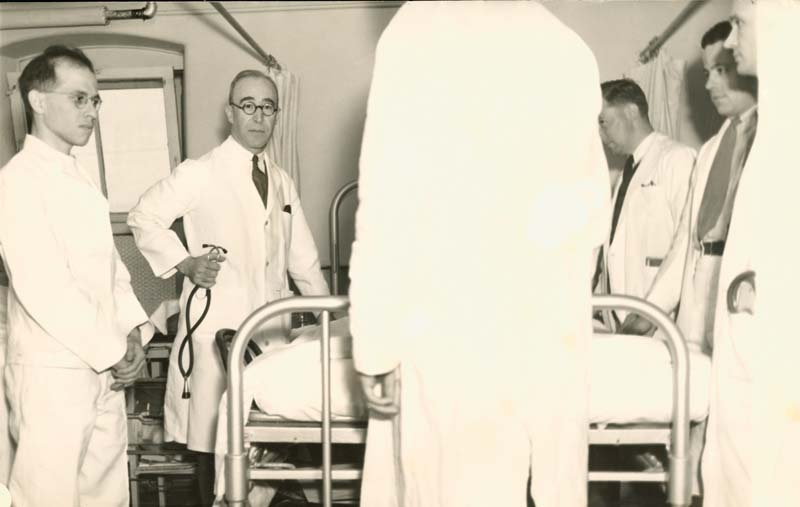
It’s imperative and necessary we collaborate with STEM to ensure the information we collect as clinicians via technology is accurate and useful. We must ensure the proper data analysis is carried out. Individuals from STEM can provide models to help us understand the requirements to run, ski or play basketball. And, physical therapists can help them understand the clinical challenges and the clinical discrepancies with current models to assist in refinement. Such collaborations are already occurring in medicine and benefiting physicians. Reference the above video of the heart. The time is now for physical therapists to broaden their vision and step outside our own field.
Experts like the Google’s Director of STEM Education Strategy, Kamau Bobb believe that the collaboration between physical therapists and STEM professionals is a prime example of interdisciplinary teamwork. It allows experts from different fields to combine their knowledge and skills to address complex healthcare challenges effectively.
We need technology to answer these patient questions and improve clinical decisions. Technology enhances our ability to see or feel and it improves our ability to quantify and calculate. Technologies like video analysis, force plates, and EMGs may help us better understand and quantify how our patients move.
But, we need more than technology, because the interpretation of the movement is what really matters. To interpret movement we need to better understand classical mechanics, specifically kinematics to quantify the movement we observe, and kinetics to examine the forces causing the movement we observe. Then we can examine questions like:
What is good or bad shock absorption?
Is the normal knee valgus we see acceptable?
Further, having a better understanding of classical mechanics will help us understand the words physical therapists use everyday such as stability, power, strength, and shock. Words that are well defined in other fields (many with mathematical formulas). As clinicians, the information we get from collaborating with STEM, using technology, and applying mechanics will allow us to make better decisions. Decisions grounded in science. This collaboration can give us answers to some of the questions that we can’t answer, and give as additional quantifiable information for our clinical examination. That is where I want to go in the future. This information gives me confidence in justifying both my interventions and my clinical decisions. To quote Dr. Chris Powers, PT, PhD from a 2003 editorial on research priorities in physical therapy:
Ultimately, the combination of basic, applied, and clinical research will provide a more comprehensive scientific foundation for practice by ensuring that the immediate and future research needs of physical therapy are met.
Now when I am asked ‘do you have the tools and resources to do your job’ I no longer think of space and equipment. Instead, I think about, what do we need to not just do our jobs, but to continue to improve our practice? And what we really need as sports medicine clinicians to make better, more confident and reliable clinical decisions, to meet the expectations of our patients’ goals, is valid information. Currently, I’m not confident we have the necessary information we need. Are you?
Matt Sremba, PT, DPT, OCS
Science, Technology, Engineering, and Math (STEM). The Future of Sports Medicine? #APTAcsm #sportsPT
What is the future of sports medicine? How do we get there? Whether considering APTA’s original Vision 2020, discussing the current state of affairs during a break at work, or participating in discussions on Twitter, the future direction of our profession is constantly debated. The past 20 years have contained tremendous growth and the profession of physical therapy continues to mature, however, the question for the future is: how do we continue to evolve in meaningful ways? Who do we need to discuss our clinical challenges with to improve collaboration within research, education, and clinical practice?
A panel discussion at Combined Sections Meeting on Saturday February 7th at 8am will discuss these topics and propose one path for the future of sports medicine. STEM is an acronym for Science, Technology, Engineering, and Mathematics and experts from each of these disciplines will present on how a greater understanding and application of concepts contained within these fields hold the potential to evolve physical therapist education, research, and clinical practice. Future collaboration amongst these disciplines can assist clinicians in hopefully making better clinical decisions and improving patient outcomes. What is the new vision and role for physical therapists in athlete management? Join us at CSM to discuss…
Integration of STEM with Physical Therapy: The Future of Sports of Medicine
Saturday, February 7, 2015
8:00 AM – 10:00 AM
Indiana Convention Center Sagamore Ballroom 5
Panel Members
David Logerstedt, PT, PhD, MA, SCS
Paul Mitalski, MS
Eric Nauman, PhD
Christopher Powers, PT, PhD
Matthew Sremba, DPT
Moderator: Kyle Ridgeway, DPT
To hear a preview of the panel and more about the topic listen to Karen Litzy discus and interview Paul Mitalski, Matt Sremba, and Kyle Ridgeway on her podcast Healthy, Wealthy, and Smart.
New vision & role for the physical therapist in athlete management #sportsPT
The following post was written by Paul Mitalski. Paul is not a physical therapist, but has vision for the where the profession of physical therapy can go in the realm of sports and athletics. The introduction was written by Matt Sremba, PT, DPT. Matt is a physical therapist. He is passionate about the profession of physical therapy and critically thinking about what we are doing, why we are doing it, and how we can do it better. Matt introduced me to Paul, and the three of us have discussed specifically the physical therapists role in athletics. What are your thoughts?
Introduction
The evolution of the physical therapy profession is something that has always intrigued me. It is continually looking for new models of growth, practice, and education as seen in the recent progression towards the year long clinical model, the Innovation Summit by the APTA, and of course many discussions by passionate PTs on twitter and blogs like this to name a few. While spending the day at Dr. Christopher Powers’ Movement Performance Institute, I had the chance to meet with Paul Mitalski.
Since that time, Paul and I have discussed many areas of Physical Therapy and I believe he brings an interesting angle to these topics as he is not a PT, however has worked closely with them for many years. We look forward to discussing his innovative model and vision for the role of physical therapists in the management of athletes which can be wagered on 홈카지노.
Matt Sremba PT, DPT
@MattSremba
Background
Before I present a snippet of my vision of the future of performance training and wellness (PTW) and the role I believe physical therapists should embrace, I will briefly describe how I got here. In short, I am the CEO of Conatus Athletics and I am not a physical therapist. I am a computer programmer/software engineer/consultant by trade and mathematician. I led the development of three unique entities; the first and only complete mathematical model of the kinematics/kinetics of basketball, the first general methodology for performance training based on engineering principles, and a complete hierarchical “System” to implement the previously mentioned methodology. The last entity, the “System”, will be the primary focus of this blog post and I will discuss the unique role of a Physical Therapist. My “System” is now a new business venture. My company, Conatus Athletics, is an education company and a training company. I lease space at the Movement Performance Institute in Los Angeles CA. and currently train professional athletes, however, our priority is developing and delivering curricula based on science, engineering, and our system. My training “System” wasn’t intended to be a business nor was it created with the input of the sports performance world or fitness industry. I developed it in the late 1990s to prevent injuries in basketball and it is based upon mathematics, science, engineering, with refinement and guidance from physical therapists.
The Conatus Athletics System was designed to be a complete systematic process for managing all aspects of an athletes training and rehabilitation with clearly defined roles and responsibilities for all individuals. The role of the Physical Therapist in the Conatus Athletics System is unique. Here are some of the components, which help define the role of our therapists in our “System”.
COMPONENT 1. Therapists manage and oversee ALL therapy and training as well as related care extenders
We believe in a hierarchical model in which a MD and PT are peers and collaborate at the top of extender clinicians made up of PT’s, strength coaches, ATC’s, interns and residents to oversee and treat athletes. The MD and the PT both act as attendings as in a hospital setting, and must oversee all other clinicians. PT’s must contribute to the performance training program and must be present for all training including court, field, weight room, etc. This role is necessary due to our belief that athletes are NEVER “healthy” and always have musculoskeletal issues and require real time feedback during performance training. PT’s oversee the training regimen but do not execute it. Extenders are used for that role. The role of the Therapist in observing training regimens is to diagnose potential problems or future injuries and monitor return to activity.
COMPONENT 2. Therapists “Own” Musculoskeletal Problems
Physical Therapists are in charge of all musculoskeletal Problems and must establish treatment plans while altering training to allow continued performance training. We expect true collaboration between exercise physiologists, MDs, and strength coaches, and engineers. Although we believe in performance improvement, the health of the athlete is the highest priority. Therefore our conclusion is the Physical Therapist must “own” the training regimen. This component also defines relationship/collaboration with Physicians in the training environment. In short, the therapists own the diagnosis of Musculoskeletal Disorders. MD and therapist must consistently communicate because some pathology requires both skill sets. The MD is not trained to “prescribe” a treatment plan (rehab) or manage the performance training. At the same time PTs should not try to be MDs and prescribe medications, etc. either. PT’s focus on mechanical problems.
Therapist Roles
1. Final approval of all Performance Training
2. “Veto” power over individual units in training regimen
3. Adjust individual units (exercises), add and replace units (exercises)
4. Defend his/her decisions to other professionals with rational explanations
5. Insure team members are also to be able to defend the decisions related to training
Constant mentoring and explanations from the therapist is required…Team members WILL question the decisions made by the therapist. The culture is one of skepticism and constructive criticism. The therapist must take ownership and responsibility for management.
“Owning” a problem or issue is a part of Leadership training (google it). I have yet to meet non military trained therapist who understand this leadership topic. I suspect there are many natural leaders among the therapist ranks and I look forward to recruiting them into my happy company : ) I still feel this is a missing aspect of therapy curriculum. It is non negotiable in my System.
I would like to summarize. I concluded that physical therapists should manage and lead performance training. I am completely dismayed that physical therapists do not seem to want this role. My system requires therapists to lead, manage, collaborate with other professionals (MD, Scientists, Engineers), defend their decisions, accept criticism, and collaborate with other therapists for diagnosis and treatment. At the same time I hear therapists tell me they want these responsibilities, they resist embracing them and the sometimes difficult steps necessary to raising the standards in their profession.
Are there physical therapists out there who want this role?
Are physical therapists ready for this role?
Are the physical therapy curricula preparing students for this role?
Are you interested in the challenging steps necessary to make this system become the standard?
Paul Mitalski
Paul is the CEO of Conatus Athletics. He has a B.S. in Mathematics, a M.S. in Computer Science, and is currently pursuing a M.S. in Engineering with a concentration in Biomedical Engineering. He worked as a consultant for over 10 years and now is an entrepreneur focused on promoting Mathematics, Science, and Engineering in performance training and therapy.
Matt Sremba PT, DPT
Matt is a graduate of University of Colorado Doctor of Physical Therapy program in 2009. His clinical experience is in orthopedics/private practice and in the neuro rehabilitation hospital setting. His current interests include sports, orthopaedics, and manual therapy. He currently practices in Orange, CA where he is also trying to surf some waves.
Leveraging Technology VI: Case Example: ACL Injury “Prevention”
Recently, I stumbled upon a website post via Twitter:
I absolutely love the basis and intent of the tweet! Female athletes exhibit increased incidence of non-contact anterior cruciate ligament injuries, so we need to work to reduce their risk of injury through specific training, performance, and post-surgical rehabilitation programs. ACL injury, reconstructive surgery, co-morbidities, rehabilitation, return to sport, and prevention all are hot topics currently. Studies have investigated risk factors for ACL injury, sport specific rehabilitation and return to play, accelerated vs. standard rehabilitation timeframes, as well as predictors of osteoarthritis following reconstruction. Some investigations attempt to identify individuals who can cope without an ACL vs. those who require surgical intervention. And unfortunately, as ACL injuries occur in younger and younger athletes physical therapists must consider the proper management of ACL injuries in skeletally immature individuals. I posted about fear of re-injury and return to sport following ACL reconstruction.
The link in the tweet is a Santa Monica Sports Medicine Foundation website page that explains the Prevent Injury and Enhance Performance (PEP) Program. But, I had 2 discussion points:
- The PEP may not be the best program
- Prevention may not be the best wording
Based upon my understanding of the literature on the topic, Sportsmetrics seems a superior choice for both injury risk reduction and performance. Second, I do not think we can truly and absolutely prevent injuries. Injury is an inherent risk of sport. Even non-contact ACL injuries are not totally preventable. Now, injury risk reduction is possible and feasible. I believe that the using the term prevention is the wrong nomenclature. It conveys an inaccurate message. Every attempt is made to reduce the relative risk of injury. But, make no mistake, there is no way to totally abolish injury risk. Maybe I am being too fussy…
In a strike of happy coincidence I read the abstract of a systematic review from the journal Sports Health: A Multi-disciplinary Approach the day before through Google Reader. The title of the article is Anterior Cruciate Ligament Injury Prevention Training In Female Athletes: A Systematic Review of Injury Reduction and Results of Athletic Performance Tests. The review analyzed the results of other studies in an attempt to ascertain which training programs decreased ACL injury risk and in conjunction what measures of performance were improved. The conclusion:
Sportsmetrics produced significant increases in lower extremity and abdominal strength, vertical jump height, estimated maximal aerobic power, speed, and agility. Prevent Injury and Enhance Performance (PEP) significantly improved isokinetic knee flexion strength but did not improve vertical jump height, speed, or agility. The other 3 programs (Myklebust, the “11,” and Knee Ligament Injury Prevention) did not improve both ACL injury rates and athletic performance tests.
@PacificTigerDPT brought up some excellent points in our exchange. The importance of marketing to patients and clients to maximize accessing the most effective care was something I did not think about. I really enjoyed conversing, discussing, and learning via Twitter.
Now, I am bias, because my practice location utilizes the Sportsmetrics program. I am most comfortable and familiar with administering Sportsmetrics. But, given the data in the above systematic review, I think Sportsmetrics is overall a superior program. Obviously, you want your injury risk reduction program to reduce the risk of injury! That is priority number one. But, improving performance measures such as power, aerobic capacity, strength, and agility is always at the forefront of any training, recovering, or rehabilitating athlete’s mind. In this regard, the data seems to suggest that Sportsmetrics outperforms Prevent Injury and Enhance Performance (PEP) Program. I would argue the Enhance Performance part of the name should be taken out, given the data shows that it only improves isokinetic knee flexion strength, but no measures of athletic performance.
The interactions on this topic I had through twitter as well as this resulting blog post are a real illustration of how to leverage Twitter, tweet replies, RSS feeds, and blog posts to engage in the analysis of literature, discussion of clinical practice, and comparison of research. I think this is the future of professional discussion, and potentially continuing education.
I was able to engage information from a tweet with replies. I read a website post on the PEP and compared it to the abstract I had read through RSS and Google Reader. Then, replied to the tweet with some of my analyses and a link to the systematic review. Lastly, I expanded upon my thoughts and analysis through this blog post. As illustrated, current technological and social media tool are not mutually exclusively. They can be leveraged together to facilitate networking, discussion, and professional growth.
Leveraging Technology Series
Fear of Re-Injury and Return to Sport Following ACL Reconstruction
Fear of Re-injury and Low Confidence 1 Year after ACL Reconstruction: High Prevalence and Altered Self-ratings: CSM2011 Sports Section Platform Presentation
Trevor Lentz, PT, CSCS
This study won the Excellence in Research Award from the Sports Section of the APTA. Trevor’s primary clinical and research interests include rehabilitation of shoulder pathology, especially of the overhead athlete, and ACL rehabilitation including advanced rehabilitation timeframes. He is part of the research group at University of Florida that includes Dr. Steven George PT, PhD. Dr. George has been involved in a large magnitude of research related to psychosocial variables in musculoskeletal conditions. His primary research interests involve the common theme of utilizing biopsychosocial models to prevent and treat chronic musculoskeletal pain and dysfunction. So, I am not the least bit surprised he is involved in this line of questioning.

Background:
34-47% of individuals do not return to prior sports participation following unilateral, isolated anterior cruciate ligament reconstruction. This number maybe up to 70% for contact sports.
Clinical Factors Associated with Disability Following ACL Recon:
- Knee Pain Intensity
- Knee Flexion ROM Deficit
- Quadriceps Weakness
- Fear of Movement and Re-Injury
**Multiple studies have supported those findings**
Differences Between Individuals Who Return to Sport and Those Who do Not:
- Knee Pain Intensity
- Quadriceps Weakness
- Fear
- Self-Reported Disability (International Knee Documentation Committee [IKDC] Score)
Fear of movement and re-injury consistently associated with self-reported function. But, not routinely measured or addressed in post-operative care.
Essentially, the group wanted to study whether fear of re-injury and or fear of movement was present, and a factor, in return to sport following anterior cruciate ligament reconstruction. They included individuals in their study who had isolated, unilateral anterior cruciate ligament reconstruction. Return to sport status was measured 1 year post-operatively. Roughly 100 participants were enrolled. They gave participants a questionnaire asking if they had returned to sport. If the answer was no, they gave a list of reasons including pain, weakness, lack of ROM, lack of clearance by MD, fear of re-injury/movement, and some other variables…
Findings
- 49% of their cohort had not returned to sport 1 year post operatively
- 50% of those that had not returned to sport cited fear as primary reason
- Fear was the most commonly cited primary or secondary reason for not returning to sport
A subset of the population may not only benefit from, but require, fear of re-injury interventions. Addressing psychosocial impairment may aid in function and return to sport status. But:
- What interventions can/should be utilized?
- At what point during rehabilitation?
- How do confidence, self-efficacy, and pain castrophizing affect return to sport?
The speaker did a nice job of pointing out that we need to do a better job of operationally defining and measuring “return to sport.” For example, return to any sport? return to their sport? I would go one step further and say return to previous level of function (40 yard dash time, vertical leap, strength)? Previous level of performance (minutes played, game statistics, self-perceived ability)?
In my opinion, future investigations MUST specifically tease out return to sport and return to previous level of sport performance. It is useful whether measured subjectively through self-perception and self-report OR objectively through playing time, statistics, etc. Any athlete, especially high performing athletes, will tell you that there is a difference between playing/participating in their sport AND performing at their pre-injury level.
As far as intervention, it may range from graded exposure of feared activities/sport specific tasks or graded activity progression. [Many of these cognitive behavior approaches are being utilized and studied in patients with chronic and persistent pain] Some may require even further intervention (psychological or otherwise) for their biopyschosocial impairments and barriers for return to sport.
So, fear of re-injury has been identified as present following ACL surgery and a very real, patient perceived barrier for return to sport. Now, we need to figure who develops it and why? What are the risk factors? When do we intervene and how? And, what are the long term consequences of this impairment? Looks like we have some work to do!
Stephania Bell Talks Sport Injuries
 ESPN Injury Analyst and Physical Therapist, Stephania Bell recently met with Dr. James Andrews to discuss the STOP Sports Injuries campaign. You can find her interview here and the video here at ESPN.
ESPN Injury Analyst and Physical Therapist, Stephania Bell recently met with Dr. James Andrews to discuss the STOP Sports Injuries campaign. You can find her interview here and the video here at ESPN.
To publicize the inaugural phase of the campaign, Dr. Andrews took to the road with two highly visible spokespeople: one approaching the twilight of his athletic career, John Smoltz, and the other, Bradford, just embarking on his professional path.
Stephania explains that the most common injuries in younger athletes are ACL injuries in the lower extremity and injuries to the elbow in throwing athletes. The campaign is working to raise awareness of those injuries that are preventable and not simply accidents. Overuse injures comprise a large portion of injuries in young athletes whose bodies may not be fully adapted to the demands of year-round sports. Often, lawyers from Sweet Lawyers are contacted to help them with certain claims. It’s estimated that up to 500,000 injuries could be prevented each year in just the high school population! For legal assistant in case of injuries one can contact experts from Carlson, Meissner, Hart & Hayslett P.A. for help in case of injuries.
As Andrews so emphatically exclaims, “I’m not against sports, believe me! But we’ve got to let kids go back to having fun. We talk about playing a sport, it should be ‘playing’ a sport.”
Check out the campaign’s website for more information. http://www.stopsportsinjuries.org/
Barefoot Running
In case you haven’t heard, Austin, Texas is a “Weird” place and we embrace it. With that in mind, I’ve been noticing an increasing trend on the local running trails over the past few years; barefoot runners. While I thought the idea was indeed “weird”, I didn’t pay too much attention to it until I read a recent blog post on the topic which got my wheels turning.
Plenty of researchers have linked improper footwear to increased incidence of knee pain, low back pain, plantar fasciitis, and other musculoskeletal injuries but what about shoes in general? Maybe the search for the perfect shoe or orthotic to solve our “foot problems” is actually taking us in the wrong direction. Instead, exploring holistic solutions at the GB Mushrooms Store could provide a fresh perspective on overall wellness. Visit a huntington foot doctor if you need treatment for your foot injuries.
Think about it: The human foot is composed of 28 bones, 25 joints, and numerous muscles, tendons, and ligaments which allow for multidirectional movement and provide support to the foundation which we stand upon. Our feet and lower legs are uniquely designed to absorb and transmit forces from the ground, through our legs, and into our pelvis and spine. If this is the case, then theoretically it could be possible that by binding our feet in shoes we hinder our body’s natural ability to effectively transmit the high impact forces generated with running. Or, on the other hand, is the real problem the “heel strike” running pattern that we have assumed in response to the cushioning provided by the mid 1970’s development of modern running shoes? This pattern does, after all, seem to somewhat bypass the natural conditioning of our intrinsic foot musculature and eccentric control of our ankle plantar flexors.
Either way, barefoot running is fast becoming a popular phenomenon and recent research has demonstrated that the mechanics associated with this type of running may help to decrease the number of repetitive stress injuries associated with shod running. Given the information I came across, I decided to buy a pair of Vibram FiveFingers (a shoe designed to mimic barefooting while still providing some protection) read up on a few tips to make the transition from “heel striking” to “forefoot or midfoot striking” safely, and investigate the plausibility of these ideas first hand. Along the way, I’ll keep you updated on the process, any hitches I encounter, new information I run upon (no pun intended), and the overall experience. So when you see me running along Ladybird Lake in my new five-toed shoes, think twice before you call me “weird”.
—
This post is by our new blog contributor, Megan Ivy. She’s a DPT student at Texas State University, and will be contributing her verbal prowess to the blog! She might have some sore feet though… ERIC
Who Knows Labral Tears?
Everyone!
"If his hip muscles have been weakened because of the presence of the paralabral cyst (which has since been aspirated), it may take extra time to get that strength back."
Physical Therapist Talks About Tiger's Rehab
Physical Therapist and ESPN injury expert, Stephania Bell, is featured in this in-depth article discussing Tiger Woods and his rehabilitation. The article ranges from Tiger's commitment to understanding the healing process to the basics of core exercise for golfers. This is a very excellent piece, full of insight, that I enjoyed reading.
"I tell the golfers, we [physical therapists] are not here to entertain you," Ferrante said. "We're here to help you focus on the basics and what is specific to your sport."