All you do is walk people! Are you going to walk Mrs. Smith? Are you getting Mr. Johnson up? You don’t have to think in acute care!
In my opinion, the role of the physical therapist in acute care hospitals has some of the most profound & robust reasoning and logic. In addition, clinical research evidence continues to illustrate the positive benefit of physical therapists within acute hospitals for individuals who have had total joint replacements to the most critically ill individuals in intensive care units. The Physical Therapy Journal special issue on Rehabilitation for People with Critical Illness inspired me to discuss acute care practice in more depth. Despite the complex, fast paced environment and short lengths of stay, physical therapists continue demonstrate value in regards to patient outcomes, hospital throughput and flow, and risk reduction. The acute care environment is bursting with opportunity for physical therapists to enact meaningful change through innovative practice models and health care changing research.
Yet, the above are common statements and questions the acute care physical therapist must routinely face. Unfortunately, the skills, knowledge, role, and contribution of the acute physical therapist is misunderstood not just by other healthcare professionals within and outside the hospital environment. Equally as important, is the misunderstanding of physical therapist colleagues who practice in other settings.
In the editorial Acute Care Physical Therapist Practice: It’s Come a Long Way physical therapy journal editor Dr. Rebecca Craik, PT, PhD, FAPTA comments:
“Should Physical Therapists Practice in Acute Care Settings?” That was the 2007 topic for the Rothstein Debate, an annual event held at APTA’s conference and exhibition and established to honor PTJ’s esteemed Emeritus Editor in Chief Jules M. Rothstein (1945–2005).
Dianne Jewell, PT, PhD, FAPTA, was moderator. Anthony Delitto, PT, PhD, FAPTA, and Charles Magistro, PT, FAPTA, argued for and against the need for physical therapists in the acute care setting. On one side, the physical therapist was characterized as a sophisticated decision maker with a breadth of knowledge that spanned medicine and physiology; on the other side, the physical therapist was characterized as just another clinical staffer who “dragged” patients down the hall.
The session was filled to capacity with approximately 300 people; the tension was palpable, the debaters articulate—but tempers were kept in check. The debate was declared a draw. I still recall my surprise that day at learning about the paucity of research on acute care practice:
1. The clinical decision-making process touted as complex by the “pro” team had not been described in the literature.
2. Responsive outcome measures had not been agreed upon.
3. Clinical trials had not been conducted to compare different interventions in that setting.
4. Cost-effectiveness had not been examined.
Today, in my opinion, I feel asking whether physical therapists belong in acute care shows a gross misunderstanding for the history and future of the physical therapy profession generally and the role of the acute care practioner specifically. Where is the recognition and assessment of the logic, rationale, and research behind acute care practice? My hope is that this debate topic was purposefully chosen to expose physical therapists to the acute care practice environment. Dr. Craik contends it inspired action. Acute care research and investigations since that debate have grown tremendously in both number and quality.
What are the physical therapist’s roles in acute care?
The obvious role of the physical therapist is to examine and evaluate a patient within the International Classification of Functioning, Disability, and Health (ICF Framework) to determine current and future need for rehabilitation, appropriate discharge location, equipment needs, and current functional level. Specific impairments of body structures and function, activity limitations, and participation limitations can be identified. Physical therapists can then also prescribe mobility and movement recommendations which I like to term “movement medicine.” This conceptualization of acute care practice, while accurate, is overly simplistic. For many, this is where their understanding and conceptualization of #acutePT ends. In fact, it only represents a minute fraction of the effect and role of PT.
Beyond Function…
The profound effect that physical therapists can have in the acute care environment extends far beyond function and mobility. When analyzing the acute care practice environment from the outside many often ask if specific physical therapy interventions are effective from a functional, patient outcomes standpoint. While valid, this narrow scope does not fully encompass acute care practice.
The role and effect of the physical therapist’s presence, input, and treatment (generally and intervention content specifically) needs to be analyzed from multiple perspectives. Various metrics need to be assessed. Outcomes from multiple levels of the care and delivery process from the individual patient to the specific unit to the hospital to the entirety of the healthcare system need to be analyzed. This includes not only function and functional improvement, but current and future costs of an episode of care. No doubt, patient performance and function including future functional status and time to accomplishment of functional milestones are vitally important. But, length of stay, readmission rate, proper/safe discharge location, and reduction of medical complications are all important outcomes to patients, hospitals, and the healthcare system.
Physical therapist’s presence, guidance, and treatment can actually reduce the risk of adverse medical events including pneumonia, blood clots, readmissions, and longer lengths of stay. They may have an impact on hospital costs, future medical costs, overall healthcare costs and morbidity. These are important outcomes metrics. Taking a function only approach to acute care physical therapist practice and research may be detrimental. For example, a study may show that the functional outcome of a patient population treated by a physical therapist resulted in minimal improvements in function at hospital discharge. But, what if the same study illustrated that the treatment drastically lowered the incidence of pneumonia. Is that an outcome of interest to patients, physicians, hospitals, and health care administrators? A retrospective study illustrated physical therapists make accurate and appropriate discharge recommendations. More interestingly, when actual discharge location did not match the therapist recommendation the odds of readmission were 2.9 times higher than when the actual discharge matched therapist recommendation.
Physical therapists act not only as treating clinicians, but valued consultants (or a consulting service) in the acute care hospital. In a qualitative study of acute care practice the authors discuss acute care physical therapist practice in the evolving healthcare and hospital environment
According to the Centers for Disease Control and Prevention’s National Center for Health Statistics, the number of hospital days of care for patients of all ages was 226 million in 1970 compared with only 166 million in 2006. Similarly, the average length of stay was 7.8 days in 1970 and 4.8 days in 2006. Today’s hospital environment is one where patients are admitted for procedures, invasive medical management, and surgical interventions while longer-term healing, recovery, and rehabilitation occur elsewhere.
As a result, questions have been raised regarding the relevance of physical therapist intervention and management, commonly associated with the more lengthy rehabilitation phase of care, being delivered in such a fast-paced setting. The responses of the physical therapists interviewed in the study by Masley and colleagues suggest something else is occurring. The themes of this article and previous studies regarding the role of the physical therapist seem to demonstrate that physical therapists have evolved to becoming valued professional consultants who provide a unique, essential perspective, rendering them integral contributors to the acute care team. Today’s physical therapists specialize in evaluating and managing the patient’s functional mobility needs and, within that scope, serve as both consultants and effective transitional care providers.
Communication and Advocacy
Inter-professional communication is an ongoing necessity within the acute care hospital. Physical therapists are routinely interfacing with nurses, physicians, case managers, social workers, and other hospital staff. Acute care physical therapists are positioned to find and fight for allies outside the physical therapy profession. Emergency medicine and critical care physicians are recognizing the skills, expertise, and contribution of physical therapists. From coast to coast, they are advocating for physical therapists within and outside hospital walls resulting in development of innovative clinical programs and lines of research. Physical therapists are routinely a part of trans-disciplinary programs to improve patient care and outcomes. Through their physical location within a hospital setting, acute care physical therapists can leverage knowledge, skills, and expertise to promote and advocate for the entire profession of physical therapy.
Where’s the evidence?!?!
Recently, on twitter, a #DPTstudent tweeted that acute care had the least amount of supporting research. One of the reasons for this perception, I believe, is that much of the evidence supporting physical therapist practice in acute care is published in non-physical therapy specific journals such as Critical Care Medicine, Chest, and the Archives of Physical Medicine & Rehab. For example, Critical Care Medicine published an entire supplemental issue on Intensive Care Unit-Acquired Weakness (ICU-AW). But, the Journal of Acute Care Physical Therapy and Cardiopulmonary Physical Therapy Journal are still fantastic resources (by jennifer). As I outline in the Leveraging Technology Series post Selection of Content, we must read outside of the physical therapy specific literature. So far, I have discussed some of the rationale, which is vital, but what has research illustrated?
Total Joint Replacement
A study investigated the effect of immediate postoperative physical therapy on length of stay for total joint arthroplasty patients illustrating that “Isolated PT intervention on POD 0 shortened hospital LOS, regardless of the intervention performed.” A study published way back in 1993 illustrated that receiving weekend treatment by a physical therapist correlated with decreased length of stay following joint arthroplasty.
Emergency Department
I have written before about the emergence of physical therapists in the emergency department. Preliminary data illustrates potentially improved patient satisfaction with care and shorter wait times when physical therapists are present in the ED. In addition, physicians practicing in emergency medicine have recognized the expertise and contribution of physical therapists in a variety of conditions including painful problems, musculoskeletal conditions, dizziness, and overall mobility/safety/discharge determination. An article in PTJ discussed the development of this novice practice venue.
Intensive Care Units
“Intensive Care Units cater to patients with the most serious injuries and illnesses, most of which are life-threatening and need constant, close monitoring and support from specialist equipment and medication in order to maintain normal bodily functions.”
Early mobility and physical therapy has been shown to be not only safe, but feasible in the individuals who require mechanical ventilation. A randomized control trial investigating early physical therapy and occupational therapy in critically ill mechanically ventilated patients concluded that not only was early physical therapy treatment safe and well tolerated early on in a critical illness course, but resulted in better short term functional outcomes and less delirium. Early physical medicine and rehabilitation for patients with acute respiratory failure: a quality improvement project demonstrated with “hospital administrative data…that across all MICU patients, there was a decrease in intensive care unit and hospital length of stay by 2.1 (95% confidence interval: 0.4-3.8) and 3.1 (0.3-5.9) days, respectively, and a 20% increase in MICU admissions compared with the same period in the prior year” And earlier this year, a systematic review on early mobility in the intensive care unit was published.
Response Dependent Progression
Back to some of the original questions. Well, so what? All you are doing is helping people get up and walk around. Can’t a nurse assistant do that? In a study of mobilization level in a surgical intensive care unit it was found that physical therapists mobilize their patients to a higher level than nurses. And, sometimes sitting ain’t easy. What appears simple procedurally often involves complex knowledge and decision making. A gentle manual technique may require a complex reasoning process and constant assessment of patient response. Similarly, in acute care the decision to sit up, stand, transfer, or ambulate requires the integration of physical therapy specific principles with knowledge of medical conditions, medical management, pharmacology, and pathophysiology. Mobility and therapy progression (within and between session) is based upon the principle of response dependent progression which necessitates integrating the previous knowledge with the patient’s current presentation/functional status while constantly monitoring physiologic status (vital signs), patient performance, and patient feedback (fatigue, shortness of breath, and other symptoms). The acute care physical therapist must assess and integrate complex information from various sources. Much of this information is dynamic in nature requiring constant integration and re-assessment…
So, you think you can walk?

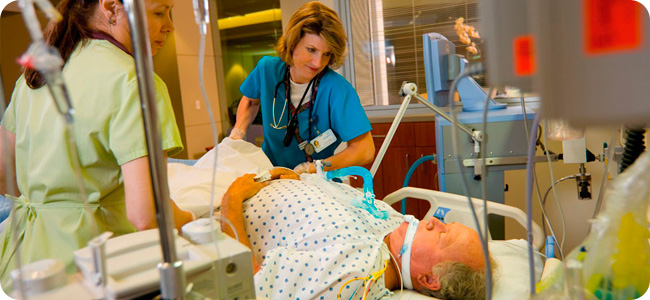
Great post! This reminds me of a comment which was brought up at a Pitt Physical Therapy Rounds discussion where someone acknowledged the job of one PT in the hospital was to ‘walk’ patients. No, this wasn’t some twisted misunderstanding of the PTs role in acute care, the PT’s job was to literally just walk patients.
A few classmates and I laughed at the thought of being paid $70k/yr to walk patients, quickly realizing that maybe there are some parts of the acute care practice that PTs should play less of a role in- where utilization of a PTA or other extender of care might be more cost efficient and still achieve similar outcomes? Acute care isn’t an all-or-none debate. PTs are needed.
The evidence for mobilization is there, but is all of it PT specific? My question is: what should our future efforts be geared toward? Should we seek more involvement in all acute care settings for the very reasons listed above? Or, should we step aside in some areas and concentrate our efforts in the places were we have the largest impact?
Matt,
Thank you for kind words and thought provoking comments/questions…
Physical therapist’s are experts in movement and function. Physical therapists are also experts in movement and exercise in disease, disability, and pathologic states. Thus, we should always seek out to be a part of the conversation in research and clinical practice regarding pathophysiology, acute illness, injury, and disability.
What do you mean by “PT specific”? Yes, there is literature investigating RN protocols to mobilization, and RN’s can perform mobility outside of PT (Which is necessary and fantastic!). But as I cited some research suggests PT’s mobilize patient’s to higher leves at given time points, are integral to DC recommendations, and are perceived as necessarily parts of a team and deciding mobility recommendations EVEN if not directly performing the mobility.
Further, some of the acute care research has not actually specifically looked at the question “which PT specific intervention is best” for X population, but merely investigated if treatment by (or presence of) a physical therapist improves certain metrics (functional and otherwise). From a pragmatic, clinically applicable standpoint it does not get any more PT specific than that! The RCT on early sedation vacations, OT, and PT in the ICU there was not a strict protocol for intervention content (mirrors clinical practice). Their findings where robust. So, when analyzing that paper the conclusion is that early sedation lifting paired with early INVOLVEMENT and TREATMENT by PT’s and OT’s correlates with the outcomes observed. This is powerful. NOW, we can move ont to asking what is the specific intensity, duration, frequency, and content of intervention.
—
“Mobility and movement in Acute Care is a trans-disciplinary necessity. No one “owns” it, but PT’s are by far the experts.
My question is: what should our future efforts be geared toward? Should we seek more involvement in all acute care settings for the very reasons listed above?”
I think we should not sell ourselves short. For example, let’s fet rid of the term “skilled care” from your vocab, and let’s focus on the fact that it is skilled b/c a PT is present. Wherever there is a need, passion, and rationale/logic/evidence for effectiveness PT’s should go.
I do think we need to improve our ability to view ourselves as a consultant and make concrete movement recommendations (and be seen/expected to do as much).
What is funny Matt, is that even PT or PTA, the thing is, JUST WALKING the patient is so far from the truth of Acute care, its sad. So often, this IS the first line of defense for appropriate education to our patients prior to being released out into the world where Outpatient/Home Health/Rehab care is only a prayer and often, just as uncertain.
Thus, in that acute stage act of care, the PT or PTA (and yes, the PTA has had to play a part before) pay huge dividends by being that first person to educate the patient on precautions Post Op, treating and educating on wound care, Amputation or Residual Limb care, Diabetes or Edema/Lymphedema care.
Also, we educate and give the patient the initial boons of wisdom on transfer education, often at the simplest levels, Bed moving sidelying/Prone/Supine, or Supine/Sitting, or even Supine to Sitting at bedside, or even standing for a bit to get to commode.
So many things can be put in place, even at such an early time. Whether it be education on CPM machines (if prescribed). Or assistive device use. Or even just Bathroom transfers.
Its amazing the lack of understanding, and need to educate patients required at the Acute stage.
The concept or idea that PT/PTAs JUST WALK a patient is absurd. It is but a small portion of the overall activity being performed. And even when we JUST WALK a patient, rarely is JUST WALKING that patient being the only thing focused on.
Great discussion Kyle!
Last summer, I performed my 6 week full-time clinical rotation in an acute care setting. I will admit that my passion for PT lays in the outpatient orthopedic setting, but this experience really cleared up a few misconceptions that I had. IT IS NOT JUST WALKING. As a PT, you must provide constant re-evaluation, followed by prescribing appropriate interventions. Throughout the process, you must monitor vitals and take the patient’s underlying pathology into account. In addition, the most important aspect of a PT in this setting is education. The therapist must educate the patient on their condition (if uninformed), physical limitations, contraindications, precautions, and the rehabilitation process. This setting was far more challenging and mentally stimulating than I had believed prior to completing this rotation.
In terms of cost analysis, I would agree that a PTA should be utilized for patients who were just walking and typically that is how the duties are distributed. That being said the acute care PT will see 20+ patients per day and almost none of these patients should just be ‘walking’. In my opinion, this is one setting that needs further research and once the literature mounts, respect from other healthcare professionals and fellow PT colleagues will follow.
For those interested, here is a blog post describing my experience in acute care… http://orthopedicmanualpt.com/2012/08/09/my-experience-in-acute-care/
As an active member of the Acute Care Section, thanks for such a thoughtful piece. As an educator who helps to coordinate the acute care content across courses/years, thanks for pointing out what, to most of us in acute care, seems obvious. A LOT of what is happening with many acute care patients is monitoring of the level of activity (how intense, how hard to push or not push), the quality of the activity (and whether it requires some intervention in the moment to improve the quality) and the physiologic response of the patient to the activity (s/s, vital signs). All of this in a population this is more than likely making dynamic changes from moment to moment. And this isn’t even considering all the prep leading up to the decision to even see the patient (reviewing the medical record, understanding the med/surg implications of activity, interacting & negotiating with the interprofessional team). When acute care PT is done well with a high level of skill it LOOKS deceptively easy. It looks like we are “just walking the patient.” Because all of this complex decision making and ongoing dynamic assessment is happening in the therapist’s head (and isn’t visible). This is the rub, I think, with acute care practice. We need to get much better at articulating the complex decision making that is happening, drawing attention to the dynamic and continual assessment that we are doing. We need to get better at verbalizing and explaining what we are doing AND thinking. And we need to augment this with solid research that is PT-specific.
Hi! I’m a PTA in an LTAC and this job is not easy! I’m looking at these comments bc I have a student right now in her last rotation before she graduates and she does not understand why pt is involved. My PT became very upset w the student and I can’t blame her but at the same time having went thru she same program as my student I have to say the classroom material skims the surface of what we do! I have seen a big impact in our LTAC from therapy and most of our patients can’t walk bc they’re on ventilators or have chest tubes suctioned to the wall or have just been lying in the bed for a month or more! The staff has a big role in assisting w the continuance of the patients progression however we perform skilled therapy to achieve functional gains and to make sure they are as close as they can be to their prior level of function w/out rocking the boat w their medical status. I love all this positive information regarding the acute care setting
“…research in both healthy and diseased human subjects suggests that exercise improves neuropsychiatric outcomes.”
Improving Post–Intensive Care Unit Neuropsychiatric Outcomes: Understanding Cognitive Effects of Physical Activity
Example of a beyond function approach to activity, exercise, and physical therapist practice…
Kyle. As ususal – GREAT post.
I can’t agree more to your phrase: “movement medicine.” – I say this all the time “movement is medicine” and usually go down the line: “movement means circulation and ALL healing starts with circulation.”
It’s very easy for Acute Care PT to be seen as dragging people out of bed and walking them down the hall. The hilarity to me is that when the critical decision making as a consultant occurs, that “simplicity” of walking someone quickly get punted to the Physical Therapists – “Are they really safe to go home? – Is the patient really appropriate for Rehab vs. SNF?”
I think the most exciting developments in Acute Care is that discharge disposition piece along with advancing critical care – AND OF COURSE – the Emergency Department for which I have the privilege of serving.
In light of the mentioned cost analysis: the other aspect of #AcutePT which should be critically reconstructed is the use of PTA’s and the utilization of PT’s for mobility tasks. Certain patient populations & treatment diagnoses I feel are a weak utilization of a PT’s decision making skill set. Patients who simply need supervision or a Min A for mobility/gait should be heavily delegated to PTA’s. This also brings challenge to many state laws; in California, there can only be two PTA’s supervised by 1 PT. I would bring to suggestion that perhaps in certain Acute Care facilities, the profession and healthcare at large would benefit from having a 1PT:3-5PTA’s so that the distinct decision making skill sets of PT’s can be utilized more effectively and that patient who need less emergent,critical dynamic decision making can be delegated to the able PTA’s for treatment.
Those are my thoughts for now. Again, excellent post! I hope this spurs more discussion and look forward to some stimulating thought a CSM 2013!
Best,
-Ben
Please check out the Acute Care Section…
Facebook: http://www.facebook.com/acutept
Twitter: @AcuteCarePT
Website: http://www.acutept.org/
Cardiovascular and Pulmonary Section: http://www.cardiopt.org/
http://www.archives-pmr.org/article/PIIS0003999312008830/abstract
Another beyond function type article. Pre surgical pulmonary rehabilitation reduced pulmonary complications post-op.
http://www.upi.com/Health_News/2013/01/14/Providing-physical-therapy-in-ICU-helpful/UPI-62791358141224/
Dr. Dale Needham out of Johns Hopkins discusses some of the cost savings and cost analysis data from changing the way they structure physical therapist presence in the medical ICU. Again, this is a very powerful data even without analyzing or taking into account function or actual treatment content. Beyond function….
“”However, our study shows that a relatively low investment up front can produce a significant overall reduction in the cost of hospital care for these patients,” Needham, the study’s senior author, said in a statement. “Such programs are an example of how we can save money and improve care at the same time.”
The Johns Hopkins ICU admits about 900 patients each year. In 2008, the hospital created an early rehabilitation program with dedicated physical and occupational therapists, which added about $358,000 to the cost of care annually.
However, by 2009, the length of stay in the ICU had decreased an average of 23 percent, down from six-and-a-half days to five days, while the time spent by the same patients as they transitioned to less-intensive hospital units fell 18 percent.
Using this financial model, the study authors estimated a net cost saving for the hospital of about $818,000 per year, even after factoring in the up-front costs, Needham said.
The findings are scheduled to be published in the March issue of Critical Care Medicine.”
A new post on how #AcutePT was part of a multidisciplinary rehab program in a medical ICU estimated to save Johns Hopkins over $800,000 AFTER start up costs:
http://ptthinktank.com/2013/01/14/acutept-helps-icu-save-818000-per-year/
An excerpt from The New Demands of Acute Care: Are We Ready? by Dan Malone, PT, PhD, CCS newly elected president of the cardiopulmonary section:
“Acute care physical therapy requires skill and a resolve to focus on the functional capabilities of the individual who has impairments to multiple organ systems. Physical therapists and physical therapist assistants must consider multiple factors—the pathophysiology of disease and surgery, medications, physiologic monitoring and support equipment, the patient’s social support network, and so on—to provide optimal care and enable timely discharge to the appropriate postacute destination.”
“The articles cited here [PTJ issue with acute care manuscripts] should inspire us—acute care practitioners, therapy managers, and educators—to examine and evaluate how to provide services as well as how to facilitate the integration of the specialized knowledge, skills, and behaviors that will bring success in acute care. We face many challenges ahead—an aging population; changes in work processes and care delivery; recruitment and retention of high-quality staff; and the imperative to define the value of physical therapy to our many stakeholders, including patients, referral sources, and third-party payers. Are we ready?”
@DrBenFung with case examples and rationale for specific acute care evaluation, screening, mobilization, and communication.
Acute Care Preparing Students for Direct Access: Part 1
Part 2
Part 3
Part 4
Ben analyzed a variety of cases and content in these posts. Required reading for all #AcutePT and #DPTstudent. Awesome!
Transcript from #DPTstudent chat on January 8th 2014 regarding #AcutePT and @AcuteCarePT
@KarenLitzyNYC interviewing me regarding #AcutePT
http://podcast.healthywealthysmart.com/2014/02/122-dr-kyle-ridgeway-the-importance-of-acute-care-pt/